
So in squamous tumors, we don’t use pemetrexed, so we would use carboplatin-Taxol, or now we use the nab-paclitaxel.
KEYNOTE 189 PLUS
Yeah, well, KEYNOTE-407 is a study presented at ASCO in 2018, which is now looking at chemotherapy plus immunotherapy in patients who have squamous tumors. In most cases, I think better tolerated than the other drugs, but in a few cases it can be quite horrific. And with targeted therapy, you tend to get gut-related and stimulated-type toxicities. So there are toxicities there, but you’re not seeing the cytotoxic toxicities that you see with chemotherapy. But most of the time it’s just mild, maybe some diarrhea, maybe some mild pulmonary infiltrate. Basically, anything that has -itis next to it can happen: pneumonitis, carditis, colitis, inflammation of different organs. You can have pretty severe toxicities in some patients, but it’s fewer than 5% who get the grade 3 or 4 really bad toxicities. Immunotherapy has different toxicities from chemotherapy or targeted therapy. And now immunotherapy-yes, a big wave of new results and data. Yeah, I think what we’ve seen over 20 years, of course chemotherapy and moving chemotherapy to early disease, then we saw the targeted therapies, starting with EGFR and then everything that’s come behind it accelerated because of the sequencing and the profiling that’s been done. So these are the patients who can’t get an EGFR, an ALK, or a ROS1 inhibitor.
KEYNOTE 189 DRIVER
And I can tell you, I’ve been taking care of lung cancer almost exclusively for more than 20 years, and this really is paradigm shifting, especially given that most of these patients do not have driver mutations. At 1 year, 38% of the patients are progression-free, but the rest have progressed, meaning there’s got to be something better. Both at our main campus and throughout the care centers, that’s being used. But right now that has become the standard of care for the nonsquamous patient, and we’re using it at Yale Cancer Center, where I work. I think in the next months we’ll start seeing some more of those data emerge. We’re still trying to investigate exactly the biology of what’s happening when you give chemotherapy plus immune therapy. So now you do maintenance therapy and pemetrexed with pembrolizumab. The use of pemetrexed as a maintenance has been shown to be quite promising and active. So usually 4 cycles of chemotherapy, these are data from many years ago and that have continued to be held up 4 cycles of cytotoxic chemotherapy are enough. Chemotherapy is active and kills dividing cells, but there are dividing cells in the bone marrow, and in the hair, and in the lining of the gut. Well, you know, the human body can tolerate only so much chemotherapy. In those patients who are PD-L1 high, more than 50%, there would still be a discussion of trying to use the immunotherapy alone. So the data looked a little bit better for the PD-L1 high than the low and the 0, but the hazard ratios for survival were significant in all 3 groups.īased on that study for the most common type of lung cancer, non-small cell lung cancer, of which nonsquamous is the most common type of that, most people would use, after discussion with patients, pembrolizumab with carboplatin-pemetrexed. But importantly, it was also positive across all lines, at least in the first analysis that was presented at the AACR in 2018. And this trial, of course, was highly positive at its primary end point with hazard ratios in the 0.6 range. So carboplatin-pemetrexed and pembrolizumab. And the study takes patients, no matter what their PD-L1 status, and treats them with chemotherapy and carboplatin-pemetrexed because they’re all nonsquamous patients or chemotherapy with pemetrexed and pembrolizumab. But even there, the response rates are less than 50%, although the results are quite extraordinary.
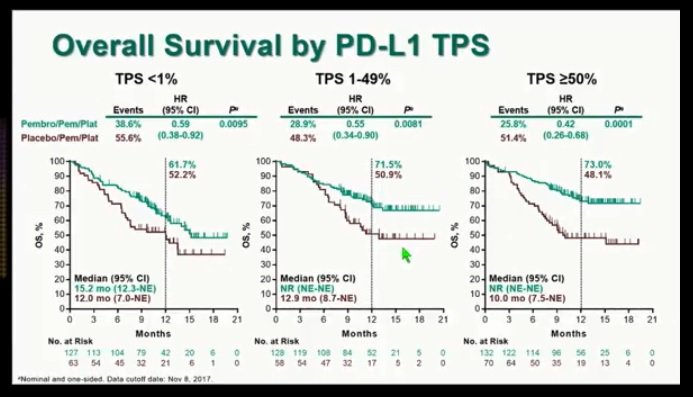
Roy Herbst, MD, PhD: KEYNOTE-189 is an important study because it took pembrolizumab, which we know can be used as a single agent in people who are PD-L1 high.
